Gut health, Probiotics and the covid vaccine Research & study
Evidence so far:
- People with poor gut health are more likely to get worse acute covid and then get long covid
- Most people’s gut get adversely effected after covid
- An intervention with yourgutplus+ and phyto-v improved outcomes after covid
- People with suboptimal gut health get more side effects and less benefit after the covid vaccine
- People to took probiotics, vitamin D and exercised had a better outcome to the flu jab
A randomised double blind placebo controlled trial evaluating the influence of gut health, vitamin D on tolerance and antibody titres post Covid-19 vaccination
EudraCT number: 2021-002826-26
 Purpose: The hypothesis for this double blind placebo controlled randomised trial is that lifestyle advice to promote gut health, supplemented by a lactobacillus probiotic, inulin prebiotic and Vitamin D in a capsule could enhance antibody titres post covid-19 vaccination compared to standard care. It is believed that higher antibody titres confers greater immunity against covid-19 exposure [Ng].
Purpose: The hypothesis for this double blind placebo controlled randomised trial is that lifestyle advice to promote gut health, supplemented by a lactobacillus probiotic, inulin prebiotic and Vitamin D in a capsule could enhance antibody titres post covid-19 vaccination compared to standard care. It is believed that higher antibody titres confers greater immunity against covid-19 exposure [Ng].
Background: Covid-19 is an enveloped, positive-sense single-stranded RNA (ssRNA) virus belonging to the Coronaviridae family. The CoV family consists of several species and causes upper respiratory tract and gastrointestinal infections in mammals. Infections in humans range from the common cold to more severe diseases such as Middle East Respiratory Syndrome (MERS-CoV) and Severe Acute Respiratory Syndrome (SARS-CoV). Severe respiratory distress is caused by the development of excessive inflammatory pulmonary infiltrates which causes severe respiratory distress, this has been terms a cytokine storm.
Several factors have been associated with severe and fatal consequences of a covid infection including older age, male gender, obesity, diabetes and co-morbidities. It has previously been shown that dysbiosis of both gut and lung microbiota also make an individual more susceptible to viral infections and sever respiratory distress [Fanos, Dang Hufnagl, Wang, Mukherjee, Fanos]. In these laboratory and clinical studies poor gut health was linked to immune and inflammatory dysfunction causing both reduced Immunosurveillance and excess, inappropriate inflammation [Shen]. Conversely, published research has shown that patients with more severely affected respiratory symptoms often have gut symptoms for many months [Smyke, Wan].
Ways to increase the ratio of healthy bacteria in the gut include exercise; reducing processed sugar, eating probiotic and prebiotic rich foods such as mushrooms, nuts, artichokes and beans; probiotic bacteria in live yogurt, kimchi and even a probiotic supplement [Roa, Hempel]. Probiotics are live microorganisms, which when administered in adequate amounts confer a health benefit on the host [Doron, Sanders]. A study in the elderly has shown that enhancing the diet with a probiotic supplement could help reduce age related falls in natural killer cell activity [Gill]. A study from Australia gave healthy athletes a prebiotic/probiotics combination or placebo. After one year the probiotic group had less colds and as a consequence had less disruption to their training. Athletes in Australia and across the world now take probiotics regularly to help avoid symptomatic viral infections. Several studies have shown that regular intake of live lactobacilli and bifidobacteria, shortened the duration and severity of upper respiratory tract infections [ Fujita, Olaimat, Rerksuppaphol, Yeh, Lei, Fanos, Berggren, Dang, Hufnagl, Wang, Olaimat]. In 2011, a Cochrane Database of Systematic Reviews, concluded that probiotics reduced the incidence of upper respiratory tract infections [Hoa]. The benefits of a specific blend of lactobacillus probiotics is currently being investigated for patients with covid-19 a UK nutritional intervention study.
As regards boosting the effectiveness of a vaccinations, several studies have suggested exercise around the time of the vaccine and certainly being generally physically active enhances a flu vaccine response [ Schuler, Keylock, Schuler, Edwards]. Likewise a recent systematic review and meta-analysis evaluated twelve scientifically randomised studies and reported that patients taking , mainly lactobacillus probiotics with prebiotics in supplements form, were found to have higher influenza hemagglutination inhibition antibody titres after vaccination in all A/H1N1, A/H3N2, and B strains. They concluded that concomitant prebiotics or probiotics supplementation with influenza vaccination may hold great promise for improving vaccine efficacy [Yeh, Lei]. .
Better vitamin D status has also been associated with greater seroprotective responses to vaccination following Influenza vaccination [Lee]. Vitamin D deficiency continues to be common across the UK, as recently confirmed in the UK Biobank cohort [Sutherland].
Several studies have also suggested that exercise around the time of the vaccine enhances a flu vaccine response. Despites these benefits for the seasonal flu vaccine, to date no study has linked probiotic use, vitamin D, or exercise with a better antibody response to a covid-19 vaccine and hence the rationale for this study.
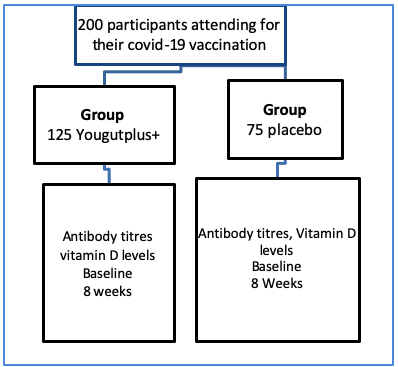 Design: After written informed consent all participants will be randomised to a nutritional supplement containing 5 lactobacillus probiotic strain, an inulin prebiotic and vitamin D3 or placebo (2:1). Both groups will also be given an information sheet to support verbal advice describing and advising the exercise, lifestyle and dietary changes which help promote health gut flora. Anti-SARS-CoV-2 Spike antibody titres will be measured at 4 weeks and 2 months in each randomised group using the Roche Elecsys®. The primary statistical end points are the difference in antibody titres at baseline and 2 months between the two randomised groups. The secondary statistical end point is the levels of exercise and BMI recorded in all participants in relation to antibody titre. Any person contracting a confirmed covid infection post vaccination also will be asked to inform the trials unit.
Design: After written informed consent all participants will be randomised to a nutritional supplement containing 5 lactobacillus probiotic strain, an inulin prebiotic and vitamin D3 or placebo (2:1). Both groups will also be given an information sheet to support verbal advice describing and advising the exercise, lifestyle and dietary changes which help promote health gut flora. Anti-SARS-CoV-2 Spike antibody titres will be measured at 4 weeks and 2 months in each randomised group using the Roche Elecsys®. The primary statistical end points are the difference in antibody titres at baseline and 2 months between the two randomised groups. The secondary statistical end point is the levels of exercise and BMI recorded in all participants in relation to antibody titre. Any person contracting a confirmed covid infection post vaccination also will be asked to inform the trials unit.
Study logistics: Data will be collected and processed at the Primrose Research Unit Bedford Hospital. Information for the trial will provided to GP’s practices, colleagues, patients groups and highlighted on social media. Any individual interested in participating will be ask to contact the trails unit before their vaccine. Participates could either be attending for their first, second or third vaccination as long as, they don’t receive the second vaccination during the four weeks of the study.
Statistical plan: Data will be collected and processed at the Primrose Research Unit Bedford Hospital. The randomization envelopes will be generated externally by research staff at the University of Bedfordshire. Once all the data has been collected the database will be anonymised, locked and sent to the external freelance statistician.
Research, development, manufacturing and quality assurance
The probiotics (Yourgutplus+) have been made specifically for this trial by an established UK manufacturers and supplied free to the trials unit by Naturemedical Ltd.
The supply companies confirm to Good Manufacturing Practice (GMP), UK and International law [www.tohc.co.uk]. They are also certified Organic by the Organic Food Federation. They have an inhouse Research and Development which measure and confirm the quality and polyphenol content of each batch for this study. Every batch is also tested for biological contamination, TBC, yeast, mould, E.Coli and Salmonella for safety. They also measure, Lead, Arsenic, Cadmium, Mercury and pesticides abiding by international threshold guidance and law.
Roche pharmaceutical have agreed to supply the antibody tests free of charge for this study
References
, et al Gut microbiota composition is associated with SARS-CoV-2 vaccine immunogenicity and adverse events
W. et al (2020). COVID-19: focus on the lungs but do not forget the gastrointestinal tract. Eur. J. Clin. Invest. 50, e13276, https://doi.org/10.1111/eci.13276
Wan, Y. et al. Enteric involvement in hospitalised patients with COVID-19 outside Wuhan. Lancet Gastroenterol. Hepatol. 5, 534–535 (2020).
Fanos V et al (2020). Lung microbiota in acute coronavirus J. Pediatr. Neonat. Individ. Med. 9, e090139, https://doi.org/10.7363/090139.
Dang, Aet al Microbes, metabolites, and the gut–lung axis. Mucos. Immunol. 12, 843–850 (2019).
Hufnagl K et al (2020).Dysbiosis of the gut and lung microbiome has a role in asthma. Semin. Immunopathol. 42, 75–93.
Wang, H. et al (2013). Gut-lung crosstalk between pulmonary and inflammatory bowel diseases. World J. Gastroenterol. 19, 6794.
Mukherjee, S et al . More of the gut in the lung: how two microbiomes meet in ARDS. Yale J. Biol. Med. 91, 143–149 (2018).
Schuler PB et al. The effect of physical activity and fitness on specific antibody production in college students. J Sports Med Phys Fitness. 1999;39:233–9.[
Keylock KT, et al. Higher antibody, but not cell-mediated, responses to vaccination in high physically fit elderly. J Appl Physiol. 2007;102:1090–8. doi: 10.1152/japplphysiol.00790.2006.
Schuler PB, et al. Effect of physical activity on the production of specific antibody in response to the 1998-99 influenza virus vaccine in older adults. J Sports Med Phys Fitness. 2003;43:404
Edwards KM, Booy R. Effects of exercise on vaccine-induced immune responses. Hum Vaccin Immunother. 2013;9(4):907-910. doi:10.4161/hv.23365.
Yeh TL, Shih PC, Liu SJ, Lin CH, Liu JM, Lei WT, Lin CY. The influence of prebiotic or probiotic supplementation on antibody titers after influenza vaccination: a systematic review and meta-analysis of randomized controlled trials. Drug Des Devel Ther. 2018;12:217-230
https://doi.org/10.2147/DDDT.S155110
Lei W-T, Shih P-C, Liu S-J, Lin C-Y, Yeh T-L. Effect of Probiotics and Prebiotics on Immune Response to Influenza Vaccination in Adults: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Nutrients. 2017; 9(11):1175. https://doi.org/10.3390/nu9111175
Berggren A et al. Double-blind RCT using new probiotic lactobacilli for strengthening the body immune defense against viral infections. European Journal of Nutrition 2010 Aug 28
Gill HS et al. Dietary probiotic supplementation enhances natural killer cell activity in the elderly. J Clin Immunol. 2001;21:264–271.
Olaimat A et al. Probiotics and prebiotics for COVID-19 Beijing UniversityScience of Food (2020)4:17 ; https://doi.org/10.1038/s41538-020-00078-9
Rerksuppaphol S et al. Randomized controlled trial of probiotics to reduce common cold in schoolchildren. Pediatrics International 2012;54(5):682‐7.
Fujita R et al. Decreased upper respiratory tract infections with daily intake of fermented milk: a multicentre, double‐blinded, RCT Am J of Infection Control 2013;41(12):1231‐5.
Hao Q, Dong B, Wu T et al Probiotics for preventing acute upper respiratory tract infections: A cochrane metanalysis (2015) https://doi.org/10.1002/14651858.CD006895.pub3
Rao S, Rehman S, Yu S Brain fogginess, gas and bloating: a link between SIBO, probiotics and metabolic acidosis Clinical and Translational Gastroenterology. 2018 9 (6) p 162.
Hempel S, Newberry S, Ruelaz A, et al. Safety of probiotics used to reduce risk and prevent or treat disease.Evid Rep Technol Assess (Full Rep). 2011 Apr; (200):1-645
Doron S, Snydman DR Risk and safety of probiotics.. Clin Infect Dis. 2015,15; 60 Suppl 2:S129-34.
Sanders M, Akkermans L, Haller D et al Safety assessment of probiotics for human use Gut Microbes. 2010, 1(3): 164–185.


